Epinephrine Auto-Injectors: Avoiding Accidental Injection

The Bottom Line
Anaphylaxis is a life-threatening allergic reaction, often to ordinary things like bee stings, peanut butter, or antibiotics. Life-saving auto-injectors are used to treat anaphylaxis. Use them safely to prevent finger sticks. Unintentional injection of epinephrine into fingers or hands can cause limited blood flow and injury. It sometimes requires a trip to the emergency room.
The Full Story
Anaphylaxis is a life-threatening allergic reaction that can occur quickly, within seconds to minutes, when someone has been exposed to an allergen. It is caused when the body's immune system releases histamine and other substances. The allergens that cause such a severe reaction can be as common as insect stings, foods such as nuts or milk, and antibiotics – though anybody can be allergic to anything.
During an anaphylactic reaction, the airway swells and closes up, the tongue can swell, and blood pressure drops. Other common reactions that are not life threatening may include nausea, vomiting, dizziness, hives, or rash.
Epinephrine, also known as adrenaline, is used to treat these life-threatening reactions. People who know they are at risk often carry epinephrine in a prefilled syringe called an auto-injector. They can treat themselves immediately while waiting for emergency help to arrive. Some common brand names include EpiPen®, Auvi-Q®, and Adrenaclick®.
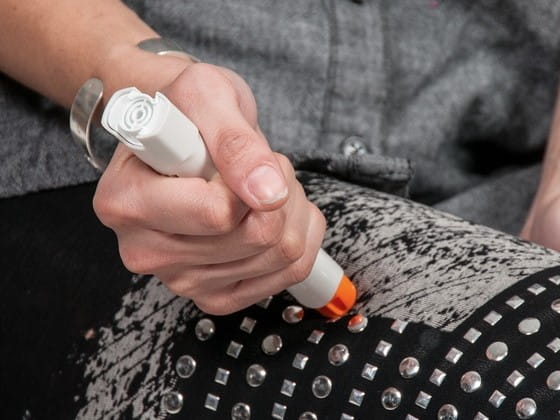
Epinephrine relaxes the airway muscles, making it easier for the person to breathe. At the same time, it constricts blood vessels, helping to improve blood pressure. Most auto-injectors contain enough solution for one dose of epinephrine. It should only be injected into the middle of the outer area of the thigh muscle when a severe allergic reaction begins.
Unintentional injection of epinephrine can easily occur when handling epinephrine auto-injectors. If the epinephrine is injected by mistake into small areas such as fingers and hands, blood vessels will constrict at the site of injection. This can decrease blood flow to the area. Less blood flow means that less oxygen is getting to the tissue. This could cause a serious injury in rare circumstances.
An epinephrine injection to a finger can cause several symptoms.
- Skin in the affected area feels cool or cold to touch.
- Skin in the affected area appears dusky, pale or even bluish in color.
- The finger or hand may feel numb or have a "pins and needles" sensation.
- Capillary refill is delayed.
- This is a quick test to determine if blood flow is diminished to a finger or toe. The nail bed is briefly pressed down until the nail turns white (blanched). When the nail bed is released, normal pink color should return within 2 seconds. If delayed, it means that circulation may be affected to that area.
- Pain and bruising at the injection site are common.
- This is not an indication of decreased blood flow and does not require emergency treatment.
If someone injects epinephrine into a finger or hand, call Poison Control immediately at 1-800-222-1222 or use the webPOISONCONTROL® online tool for help. A poison specialist (a pharmacist or registered nurse trained in toxicology) will ask a few questions. Then, he or she will tell you exactly what to do. After first aid, the poison specialist can decide if emergency room treatment is needed.
Many cases can be managed at home with simple treatment and close monitoring while being guided by a poison specialist. First, immediately soak the affected finger or hand in warm water. Or, wrap it in a warm compress, such as a wash cloth or towel dampened with warm water.
If more treatment is needed, Poison Control may recommend care in the ER. The emergency room can use other treatments.
- A vasodilator ointment can increase blood flow to the finger.
- Medication can be injected around the affected area to improve blood circulation.
- Probably, no other treatment will be needed.
With treatment, symptoms usually resolve in 2 to 24 hours. Poison Control will stay in touch with you to be sure that everything returns to normal.
Lynn Clark, RN, BSN
Certified Specialist in Poison Information
Rose Ann Gould Soloway, RN, BSN, MSEd, DABAT emerita
Clinical Toxicologist
Poisoned?
Call 1-800-222-1222 or
Prevention Tips
- Learn how to use auto-injectors. Everyone who might give the medicine needs to know how: the patient, caregivers, parents, teachers, spouse, etc.
- Keep the medication in the plastic carrying tube it comes in, tightly closed and out of reach of children.
- Most devices have a colored safety release over the needle. Keep this release on until you give the medicine.
- NEVER put your thumb, finger or hand over the needle area of the automatic injection devices.
This Really Happened
Case 1: A 15-year-old boy found an EpiPen® on a bus. He unintentionally injected the adrenaline into the tip of his thumb. In the emergency room, his thumb was cold and pale. The boy complained of pain, numbness, and tingling. Capillary refill time was five seconds, indicating that blood vessels in his thumb were constricted and limiting blood flow. He was treated by soaking his thumb in warm water and applying nitroglycerin paste to relax his blood vessels. It took six hours for complete blood flow to be restored to his thumb.
Reference: Velissariou I, Cottrell S, Berry K, Wilson B. Management of adrenaline (epinephrine) induced digital ischaemia in children after accidental injection from an EpiPen. Emerg Med J. 2004; 21:387-8.
Case 2: A 4-year-old boy found his mother's Epipen® in her travel bag and stuck himself in the thumb. The child had initial pain at the site with a small amount of bleeding. The thumb was pale and after 1 hour some bruising started to form. The mother soaked the child's thumb in warm water and massaged the area. The capillary refill was checked at this time and it was less than 3 seconds, not much longer than normal. The mother was advised by Poison Control to continue the warm soak for a short time longer and then allow the child go to bed for the night. By the next morning, the child's thumb was back to its normal color.
References
Mylan Specialty Pharma. (2012) EpiPen: Highlights of Prescribing information.
Poisoned?
Call 1-800-222-1222 or
Prevention Tips
- Learn how to use auto-injectors. Everyone who might give the medicine needs to know how: the patient, caregivers, parents, teachers, spouse, etc.
- Keep the medication in the plastic carrying tube it comes in, tightly closed and out of reach of children.
- Most devices have a colored safety release over the needle. Keep this release on until you give the medicine.
- NEVER put your thumb, finger or hand over the needle area of the automatic injection devices.
This Really Happened
Case 1: A 15-year-old boy found an EpiPen® on a bus. He unintentionally injected the adrenaline into the tip of his thumb. In the emergency room, his thumb was cold and pale. The boy complained of pain, numbness, and tingling. Capillary refill time was five seconds, indicating that blood vessels in his thumb were constricted and limiting blood flow. He was treated by soaking his thumb in warm water and applying nitroglycerin paste to relax his blood vessels. It took six hours for complete blood flow to be restored to his thumb.
Reference: Velissariou I, Cottrell S, Berry K, Wilson B. Management of adrenaline (epinephrine) induced digital ischaemia in children after accidental injection from an EpiPen. Emerg Med J. 2004; 21:387-8.
Case 2: A 4-year-old boy found his mother's Epipen® in her travel bag and stuck himself in the thumb. The child had initial pain at the site with a small amount of bleeding. The thumb was pale and after 1 hour some bruising started to form. The mother soaked the child's thumb in warm water and massaged the area. The capillary refill was checked at this time and it was less than 3 seconds, not much longer than normal. The mother was advised by Poison Control to continue the warm soak for a short time longer and then allow the child go to bed for the night. By the next morning, the child's thumb was back to its normal color.
